The Overton Window is a concept in political science that describes how the range of options from which politicians make policy choices changes over time.
When a new policy idea is introduced it may seem be radical or even unthinkable, but one effect may be that it shifts perceptions of the range of what is considered acceptable or sensible in its direction.
Things that formerly seemed out-of-bounds may seem less crazy in comparison.
While I’m not advocating mandated fasting as a governmental policy prescription, I hope what Lisa and I are doing right now might shift your personal Overton Window in the direction of at least trying a 24-hour fast before Thanksgiving.
Lisa and I are currently in the midst of our periodic #3DayCancerPreventionFast. We’re eating nothing (except Communion at church yesterday) for at least 72 hours. We are putting a small amount of cream in our morning coffee, supplementing magnesium, salt and potassium to make sure our electrolytes stay in balance, and are also drinking mineral water.
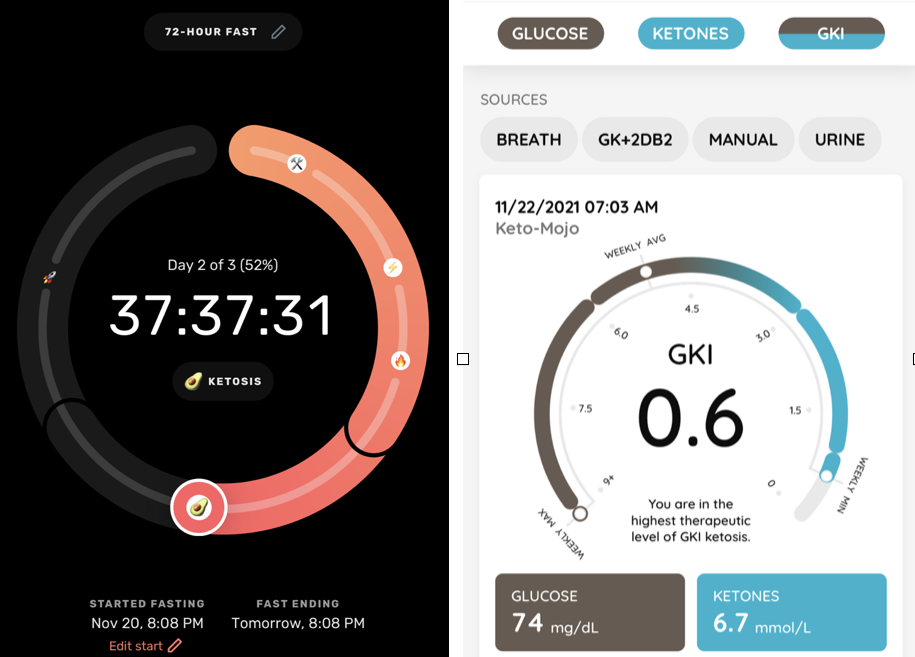
I’m just past the 38-hour mark right now. Lisa started a day earlier because on Saturday afternoon when I suggested we do this again she hadn’t eaten since Friday night, and she just decided to keep going.
Once we decide we’re going to do a three-day fast, Lisa wants to get into it and get it done. I wanted to have another bacon-and-eggs meal before I started.
Because I began my fast already having been in a high level of ketosis for a few days, I reached a glucose ketone index (GKI) of less than 1.0 by the end of the first day. Our goal is to be at that highest therapeutic level of GKI ketosis for at least 24 hours.
Lisa will end her fast tonight or wait until Tuesday morning, and I’ll finish tomorrow night or early Wednesday.
Either way, we’ll eat a few small meals to work our way back into eating mode, so we’ll be ready for a sumptuous feast on Thursday.
We’ll be able to eat anything we want without even a trace of guilt or regret.
A three-day fast may seem unthinkable or radical to you right now. It sure did to us originally, but now we’ve done it several times.
Maybe you could start with something shorter, like 24 hours. Or 18.
One person we’ve coached couldn’t imagine g0ing without eating for even eight hours. Yet by limiting carbohydrates and gradually extending her fasting window, she’s now done a 48-hour fast.
So here’s your challenge: after dinner tonight or tomorrow, don’t eat until dinner the following day.
You’ll have a prolonged period of low blood insulin levels, and you’ll be in fat-burning mode for several hours.
Then, if you’re able to have a feast on Thursday you too can enjoy it fully with no guilt or regrets. You will have paid the price in advance.
Your 24-hour fast will make ordinary intermittent fasting or time-restricted eating (fasting for 16 or 18 hours and limiting eating to 6 or 8) seem acceptable, sensible or even something you might adopt as your personal policy.
If you take the #24HourFastingChallenge, I hope you’ll leave a comment below with your thoughts on your experience and what you learned from it.